Thirty out of 78 patients (38%) had developed fluid overload due to EFT in the years preceding the study period. A history of fluid overload was a strong risk factor for a new episode of fluid overload. Fluid overload was significantly associated with a longer hospitalization period. Four patients had 2 episodes of fluid overload during the study period. Twenty (26%) of the 78 patients (13% of all 188 hospitalizations) experienced fluid overload due to EFT. Fluid overload was defined as a documented diagnosis by treating physician based on symptoms, clinical parameters or findings of lung edema on chest X-ray.Īssociation between patient parameters and the occurrence of fluid overload during a hospital admission for VOC was assessed using univariate and multivariate logistic regression analyses.Ī total of 188 hospitalizations in 78 patients were included in the study, 44 hospitalizations were in children. Patient records were thoroughly reviewed for a large variety of clinical parameters (ie fluid regimens, medical history, treatment and current or past fluid overload due to EFT). 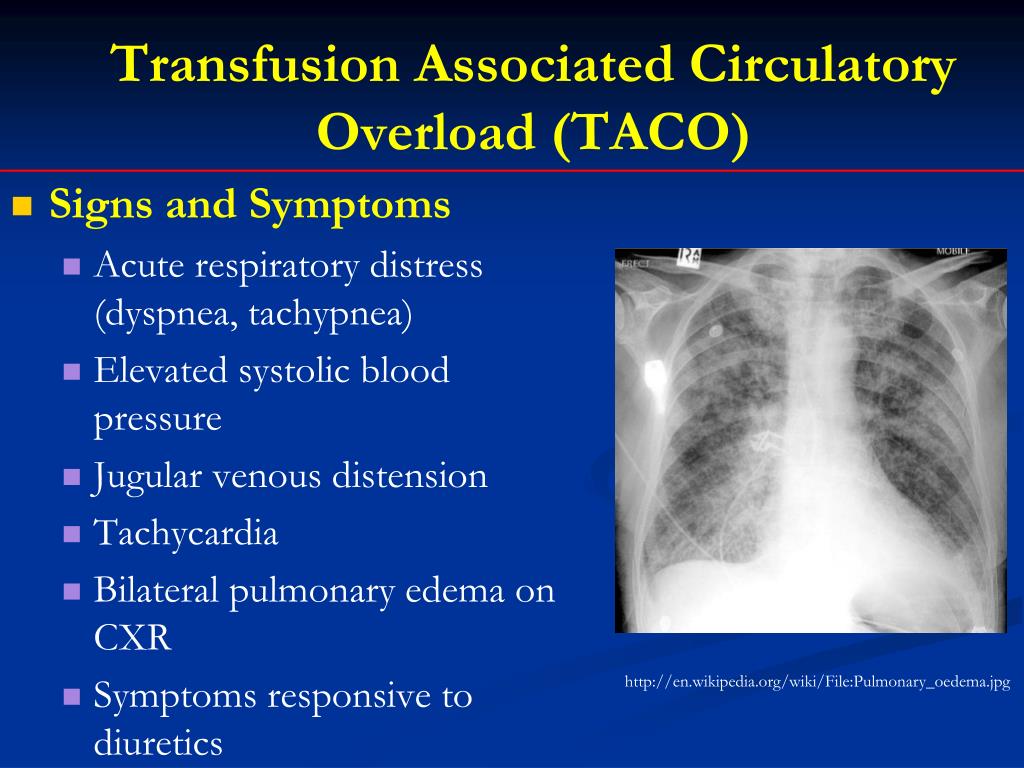
According to the local protocol, EFT existed of NaCl 0,65% 3 liter/24 hours in adults and NaCl 0.45%/glucose 2.5% 3 liter/m 2/24 hours in pediatric patients, both for the maximum duration of 72 hours. Consecutive admissions of the same patient within the study period were included. We evaluated whether fluid overload is related to fluid volume or tonicity, SCD-related complications, use of blood transfusion or hydroxyurea and laboratory parameters.Ĭonsecutive SCD patients (HbSS, HbSC, HbS-β 0 thalassemia, or HbS-β⁺ thalassemia), aged > 10 years, with a hospitalization period of at least 3 days for VOC between September 2016 and September 2018 were included in this retrospective analysis. In this retrospective analysis, we assessed the rate of fluid overload due to EFT in SCD patients. However, despite its widespread use, very little is known about the efficacy and potential complications of intravenous (iv) extra fluid therapy (EFT). Extra fluids (hyperhydration) are thought to stop or limit sickling and are therefore routinely administered as treatment of VOC, regardless of the patient's hydration state. Loss of renal concentrating capacity renders SCD patients susceptible to hypovolemia. A decrease in body fluid levels supposedly promotes the sickling process, thereby contributing to VOC. Vaso-occlusive crisis (VOC), causing severe acute pain, is the major cause of hospitalizations in SCD patients. Sickle cell disease (SCD) is a common and severe hereditary hemoglobinopathy. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
December 2022
Categories |
 RSS Feed
RSS Feed
